
Molluscum
Molluscum contagiosum is a common self-limiting viral skin infection with pus filled bumps and inflamation of surrounding skin. Mild ezcema may be present and this often makes the molluscum worse.
Mollenol can be applied when molluscum contagiosum is present to minimise the symptoms providing moisture to the skin and to counteract inflamation. You can use Mollenol as a mollusum contagiosum treatment.
Firstly, ensure you have received a medical diagnosis of molluscum from a doctor.
Molluscum is likely to be present in various stages. Use our stages of molluscum pictures to match your stage, the location of the infection and the age of the person to decide which Mollenol product to use.
Stages of Molluscum Growth
The combination of Mollenol lotion and Mollenol Patches you use will depend on your infection.
Mollenol Patches are for pus filled bumps.
Mollenol lotion is best for smaller bumps and clusters.
Extensive and stubborn bumps needs both Mollenol lotion and Mollenol Patches.
Bumps under hair and in the creases of the skin need Mollenol lotion.
Use Mollenol Sensitive for children 2-7 years and for private parts and all sensitive areas on older children and adults.
Use Mollenol standard only for adults and children 8+ years and only on non-sensitive areas.
Beginning Stage
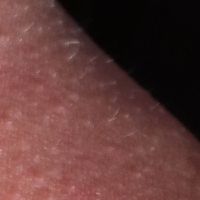
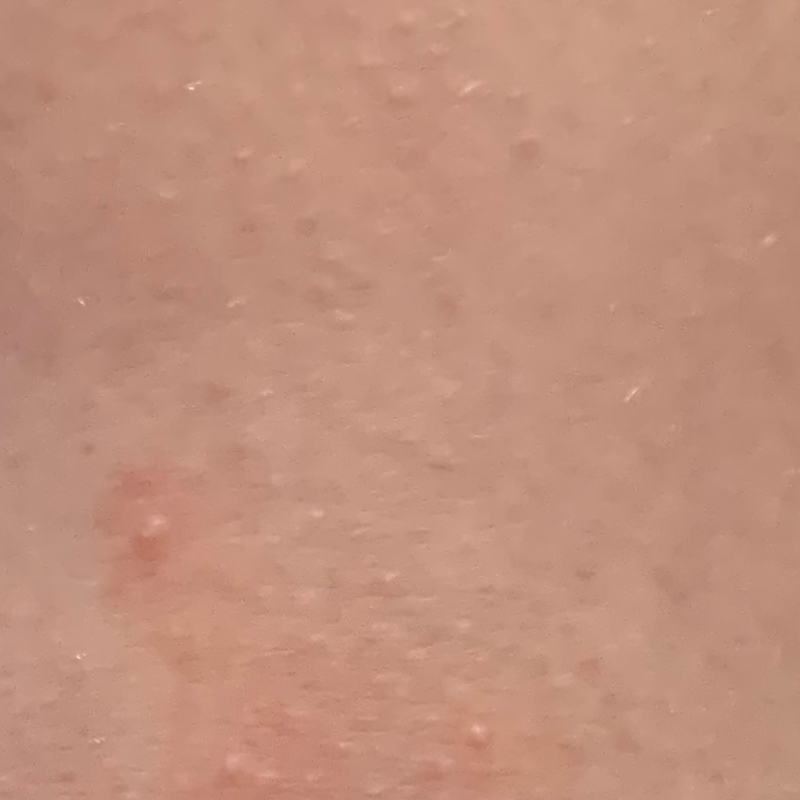
Numerous tiny skin colored bumps with three bumps swelling with pus
The stages of molluscum picture shows that the molluscum virus enters the body through hair follicles, scratches, and tiny breaks in the skin resulting in localised infection and the growth of a very small bump. 15
After an incubation period of two to eight weeks molluscum begins as tiny pin-sized white/pearly bumps often in clusters of several up to hundreds. They are difficult to see in this initial stage.
The molluscum contagiosum virus is transmitted by direct contact with an infected person or indirectly via, for example, toys, towels or clothing. Child care centers and schools as well as public pools are potential places for infection.
Which Mollenol?
Apply Mollenol Sensitive (for children and sensitive areas) or Mollenol standard to areas with beginning stage bumps. These bumps contain very little pus and Mollenol Patches are best reserved for the larger pus filled bumps.
Developing Stage
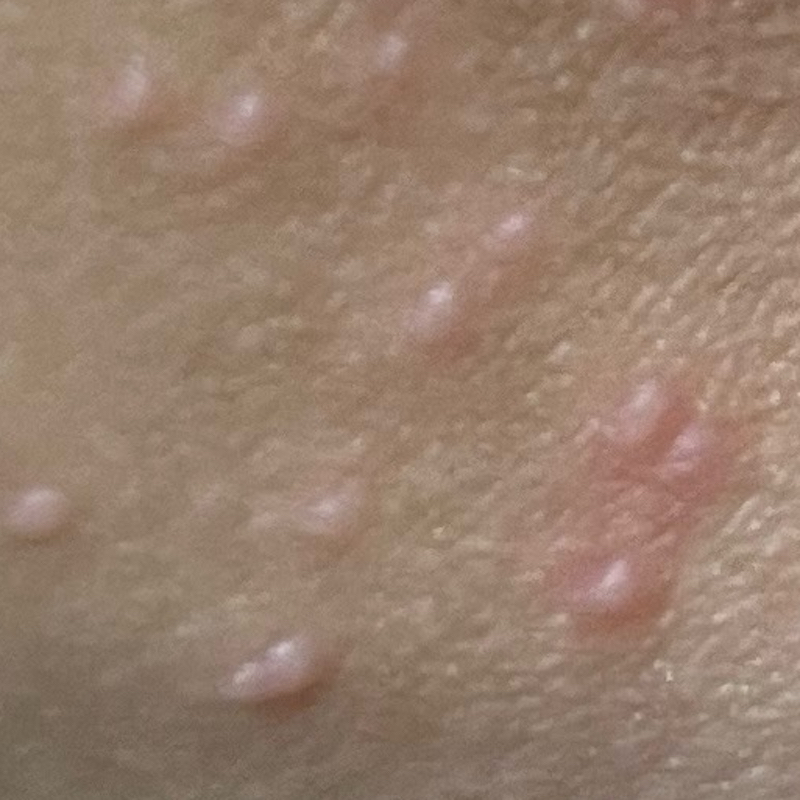
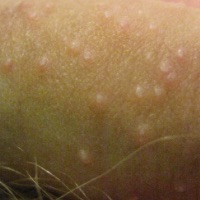
Bumps enlarging and pus growing
Over many days and weeks molluscum develops into small pearly bumps growing to 2-5 millimetres pus filled lesions often with a characteristic dimple (or dell) on the surface.16
Which Mollenol?
The symptoms associated with developing stage molluscum are best addressed by applying Mollenol Sensitive (for children), Essential Serum or Mollenol standard lotion and using Mollenol Patches for the largest bumps. After application expect to see some increased inflammation around the bumps.
Purulent Stage
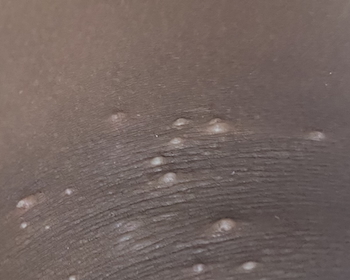
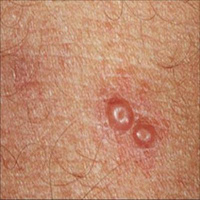
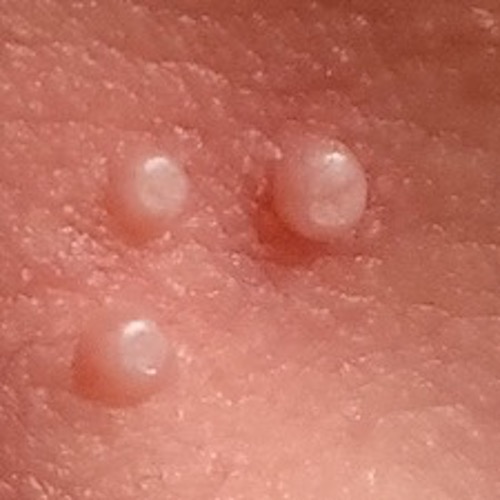
Pus filled bumps (2-3mm) with central dimple
These bumps need to be covered to limit the spread.
As the viral matter grows the pus increases and the molluscum grows larger. The dimple becomes more evident and pus may be visibly exuding.
Molluscum is now more likely to spread over the skin and to other people.
These pus filled bumps grow and then burst or open fully exuding pus.
Not controlling pus filled molluscum is how molluscum spreads.
When there are a large number of pus filled molluscum bumps about to burst extensive infection results unless preventative action is taken.
Which Mollenol?
Purulent stage molluscum are full of pus and need to be covered with a Mollenol Patch. Application of Mollenol standard lotion, Essential Serum or Mollenol Sensitive (for children) will help reduce symptoms associated with molluscum. Of course, Mollenol Patches will not stick well to hairy or creased skin, for example back of knees or neck, and these bumps will need 2-4 application of Mollenol or Mollenol Sensitive a day.
Extensive molluscum infection

Molluscum can grow and become widespread
The pus has exuded onto the body creating new molluscum.
The molluscum virus in the pus spreads the infection. Extensive spread is especially likely if pus-filled molluscum have been left for a long time, scratched or opened.
Which Mollenol?
Extensive molluscum infection has molluscum from all stages. The symptoms associated with extensive infections need Mollenol & Mollenol Sensitive and Mollenol Patches.
Burst Stage
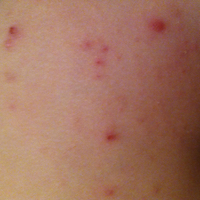
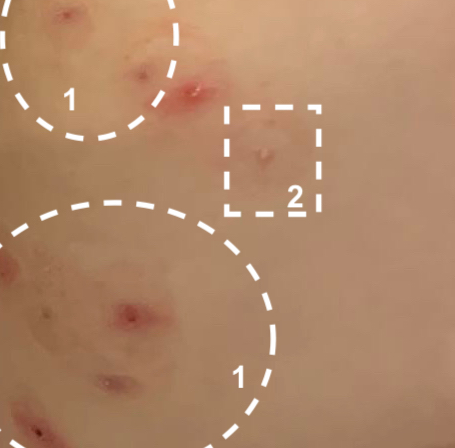
Red lesions where molluscum grew. Do not apply Mollenol lotion or Patches.
The likelihood that the molluscum infection will spread is now high.
Finally, the bump bursts (or skin breaks) and the molluscum bump transitions into a “wound” while spreading the infection. Don't apply Mollenol to these burst and open lesions as it may sting. Keep clean and covered if needed.
Molluscum which are pierced, scratched or burst run the risk of secondary bacterial wound infection. Piercing and scratching molluscum also contributes to spreading the virus.
Which Mollenol?
Generally bumps which are burst, open or scabbing (as in 1 in the photo) are no longer molluscum and should be left to heal without application of Mollenol lotion or Mollenol Patches. Keep an eye on the area as some may re-establish as molluscum or molluscum may start to grow immediately adjacent.
Don't remove the molluscum "core"
The notion of a “core” for molluscum is more misleading than useful. Molluscum are not pimples. They are a viral infection. A bump which exudes the pus will die but there are likely to be other small bumps in the area around.
Piercing, drawing or squeezing out the “core” will increase the likelihood of spread and of scarring. It also can introduce bacteria into the lesion resulting in a bacterial infection requiring antibiotics.
The pus exuding from a molluscum bump needs to be controlled. Mollenol Patches can contain the exuding. If Mollenol Patches are not used than a bandaid covering the bump will help control spread.
End Rash not hives
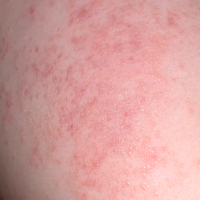
Inflamed molluscum forming a wider "rash" is the strongest response
Inflammation is usually a good sign that the immune system is fighting the virus and starting to clear the infection.
For some it is just a few molluscum, for others it is more widespread looking like a rash.
This rash is sometimes mistaken for hives. Some parents call this the “end rash”. It is also known as the BOTE, “beginning of the end”, response 18. Other medical researchers have described an id reaction as well as a Gianotti-Crosti syndrome-like generalised inflammatory reaction (GCLR) especially in atopic children presenting with molluscum and mild eczema. The GCLR reaction is potentially 5% of the molluscum infected population and usually results in resolution of the molluscum.21,22
This inflammatory response is considered a positive indication or sign of healing. It is a stage that some molluscum undergo prior to resolution, reduction, and skin healing.
An inflammatory rash can occur in areas around the molluscum as well as the molluscum itself. This is because the molluscum virus has infected a larger area than can be seen easily. A sign of this is that the rash shows up many little bumps (which look like hives) which are very small beginning stage molluscum. These bumps are inflaming and the inflammation is joining up to look like a wider rash.
Which Mollenol?
When molluscum reaches this stage only apply Mollenol lotion and Patches to molluscum which are not inflamed allowing the inflamed area to settle with many of the molluscum drying out and reducing. Essential Serum is good to have at this stage (for all ages) as it can be used to maintain the health of the skin while healing.
The Background
According to the the US Centre for Disease Control (CDC) molluscum contagiosum typically resolves without scarring but may take as long as 4 years. The lesions, known as Mollusca, are small, raised, and usually white, pink, or flesh-colored with a dimple or pit in the center. They often have a pearly appearance. They're usually smooth and firm.18
Common on the torso and thighs, molluscum can infect all parts of the body and is often associated with dermatitis and mild eczema. Molluscum generally infects children, their siblings, parents & relatives as well as adolescents, and young adults.
Molluscum is a skin virus not a blood based virus.
Research is now indicating that molluscum has unique immune evasion characteristics which may lead to persistent infections lasting months to years. The BOTE inflammatory response as an indicator of host immune activation, is the natural resolution signal. Therapeutic strategies may seek to influence the initiation of BOTE. 22
Research also shows an association between swimming, bath sharing and molluscum contagiosum. Living in close proximity, skin-to-skin contact, sharing towels, clothes, bedding, toys, and living in warmer climates are also associated with higher rates of molluscum infection.11,12
Molluscum contagiosum is more common in individuals with atopic dermatitis, and its lesions tend to be more persistent, more extensive and more generalised in atopic children. This has been reported to be as high as 49% of children in Spain under 10 years of age who were infected with molluscum contagiosum also had atopic dermatitis.
Molluscum contagiosum is a viral infection member of the Pox virus family. Also known as Water Warts or Dell Warts, molluscum is common worldwide with an estimated 170 million sufferers, 3% of the world's population.
Your Mollenol Options:
-
 SALE30% DiscountFor FamiliesUS$50.00US$69.99
SALE30% DiscountFor FamiliesUS$50.00US$69.99 -
 8yrs to AdultsStrong
8yrs to AdultsStrongMollenol 25ml (0.85 fl oz)
US$38.00 -
 ChildrenPrivate parts
ChildrenPrivate partsMollenol Sensitive 25ml (0.85 fl oz)
US$38.00 -
 NEW PRODUCT
NEW PRODUCTExtra Large Hydrocolloid Patches
US$30.00 -
 Sensitive areasRollerball applicator
Sensitive areasRollerball applicatorEssential Serum Spot Treatment
US$30.00 -
 All agesBulk Discounts
All agesBulk DiscountsMollenol Hydrocolloid Patches
US$30.00
FREE SHIPPING FOR TWO OR MORE ITEMS
